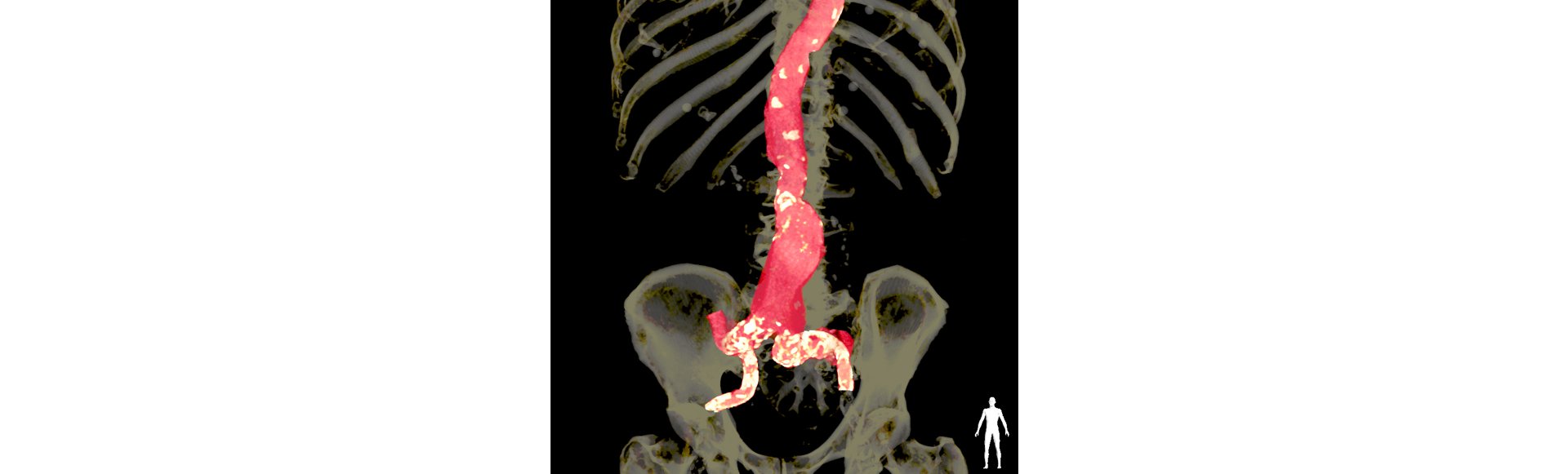
The expression ‚aneurysm` has its origin in ancient Greek. It can be translated into ‚dilation`. In medicine, a dilation of a blood vessel exceeding 50% of the normal, age-appropriate diameter, is referred to as an aneurism. Dilations of blood vessels can cause them to burst. The aim of the treatment is to prevent such rupture (Rupturprophylaxe).
Aneurysms can can affect any blood vessel of the body, however, occur frequently in certain places. So-called ‚predilection sites` include: the main artery under the thoracic diaphragm (abdominal aortic aneurysm), pelvic arteries (iliac arterial aneurysm), the main artery within the chest range (thoracic aortic aneurysm) as well as the popliteal artery (popliteal aneurysm). Splenic artery aneurysms and aneurysms in the vicinity of visceral arteries are rare. In addition to that, recognized as a predilection site for aneurysms are the arteries of the brain inside the skull (intracranial area).
The latter, however, are treated by neurosurgeons. Every now and again aneurysms appear in multiple places of the body simultaniously (Morbus aneurysmaticus). The following surgical patient information concentrates further on the description of the abdominal aortic aneurysm.
1) Cause / etiology of aneurysmal development
At a molecular level, increased activity of protein bodies in the aortic wall plays a role, breaking down the scaffold of the aorta, which consists of collagen, and thus reducing the stability of the aorta. However, what activates these proteins in the first place is still not clear, and remains a subject of research. It is known that cigarette consumption increases the risk of developing an aortic aneurysm. In addition, increased blood pressure has been proven to also promote the development of aneurysms.
2) Signs of the aortic aneurysm
This disease becomes more frequent with increasing age (increasing incidence). Usually the aortic aneurysm is symptomless and a discovery thus often results from a random incidental finding during a screening (ultrasound). Sometimes, however, the aortic anurysm does cause certain symptoms such as abdominal pain or rather pain radiating in the back or in the groin. Aneurysms are often lined inside with clotted blood components (thrombi). Sometimes thrombi particles are torn from the blood stream causing circulatory disorders (embolisms) in the legs or internal organs.
3) Diagnosis of aortic aneurysm
Throughout a clinical examination performed by a vascular surgeon, an ‘aortic anurysm’ can be detected: the surgeon senses a pulsating space requirement (increase in volume) in the mid-abdominal region. However, the clinical examination is not 100% fail-safe, so the actual diagnosis is mainly made by ultrasound, especially in obese patients. Additionally, if required, a computed tomography (CT) scan of the entire aorta (including the skull) should be performed next. Computer tomography provides information on whether the aneurysm must be treated, and, if so, how the aneurysm can be treated. Moreover, computer tomography shows if aneurysms are also present in other parts of the body.
In addition to the maximum transverse diameter, the nature of the aneurysm also determines the urgency of the treatment. Hence, the aneurysm does not always have to be spindle-shaped – it can also be saccular-shaped or even resemble a “toxic” bulge (bubble), threatening to tear. Contrast-enhanced computed tomography angiograms (CTA) also provide information on whether or not the renal arteries or the superior mesenteric artery, which supplies the majority of the small intestine, is or are affected. Lastly, CT angiography shows which type of treatment, namely open surgery or implantation of a stent graft (see explanation below) is preferred in consideration of purely anatomical reasons.
4) Aortic aneurysm treatment
Medical therapy
If the size of the aortic aneurysm is still less than five centimeters below the maximum transverse diameter and there are no other grounds for surgery, drug treatment can be effectuated, which can slow down or stop the disease from progressing. A degeneration of the aneurysm, however, is excluded. It is recommended to adjust blood pressure, that is to say, treating the hypertension. Perscribed for the stabilization of blood vessels and the inhibition of those proteins responsible for degrading the aorta support structure, are cholesterol-reducing drugs of the group statins. On top of that, acetylsalicylic acid plays an important role within the drug therapy of aneurysms, for that it stabilizes both the vessel wall and the thrombi.
Indication for surgery
As previously mentioned above, the maximum transverse diameter plays a central role. If it amounts to over 50-55 millimeters, the risk of a spontaneous, sudden rupture exceeds the risk of surgery or treatment with a stent graft. The same applies to aneurysms, that are eccentric and/or toxic.
Open operation
The open operation is performed under general anesthesia. The aorta is uncovered by means of a central abdominal or flank incision, and is clamped above as well as below the aneurysm. Next, the aneurysm sack is cut open and a plastic prosthesis is sewn in with a special technique.
Special attention must be given to the blood circulation of the kidneys – and, in rare cases, to other visceral arteries – as the aortic aneurysm may also affect the discharge of renal or other visceral arteries. The operation is technically complex and requires profound expertise, not only of the surgeon, but also of the anesthetist and other medical staff involved in the operation. Usually, patients are followed up by specialists for one to three days at a specially equipped monitoring station before they return to the normal station.
Stent graft
A stent graft is a stent made of a specially designed metal braid, which is additionally lined with plastic tissue. Corresponding its function, a stent graft can seal a blood vessel. The aortic stent is usually composed out of two components, which are advanced over the femoral artery, which is surgically exposed for this purpose, into the aorta and are unfolded there. The operation is by and large performed under general anesthesia, but can also be performed under local anesthesia if the patient would be at risk under general anesthesia.
Open aortic surgery versus aortic stent graft procedure
Until 1997, stent grafts were not routinely available. Since then, more and more stent grafts have been applied due to the technical development of the materials used. In a quarter of cases, a stent graft procedure is still not possible for anatomical reasons, so that only open surgery is possible. A perfectly performed open surgery has an equally low rate of life-threatening complications as the stentgraft.
The disadvantage of open surgery is that it is more stressful for the patient. However, according to present-day experience, the result achieved by the operation is permanent. In the case of a stent graft, on the other hand, leaks do occur from time to time – so-called “endoleaks” – which require repeated intervention (even after several years). The implantation of the stent graft is generally less stressful for the patient together with a faster healing process, so that the stentgraft is particularly suitable for elderly patients with concomitant diseases. A bothersome but rarely threatening complication after exposing the inguinal arteries for the stentgraft is the occurrence of wound healing disorders in the groin.
5) Aftercare
The first follow-up examination of the surgeon is required after six-months, then annually. Follow-ups including computed tomography are necessary after a stentgraft implantation. Even after open surgery, yearly check-ups by a surgeon are needed. In such a case, computed tomography is performed individually and as required. As with all vascular diseases, follow-ups must include an analyzis of the risk factors. Furthermore is the absence of nicotine is absolutely indispensable.