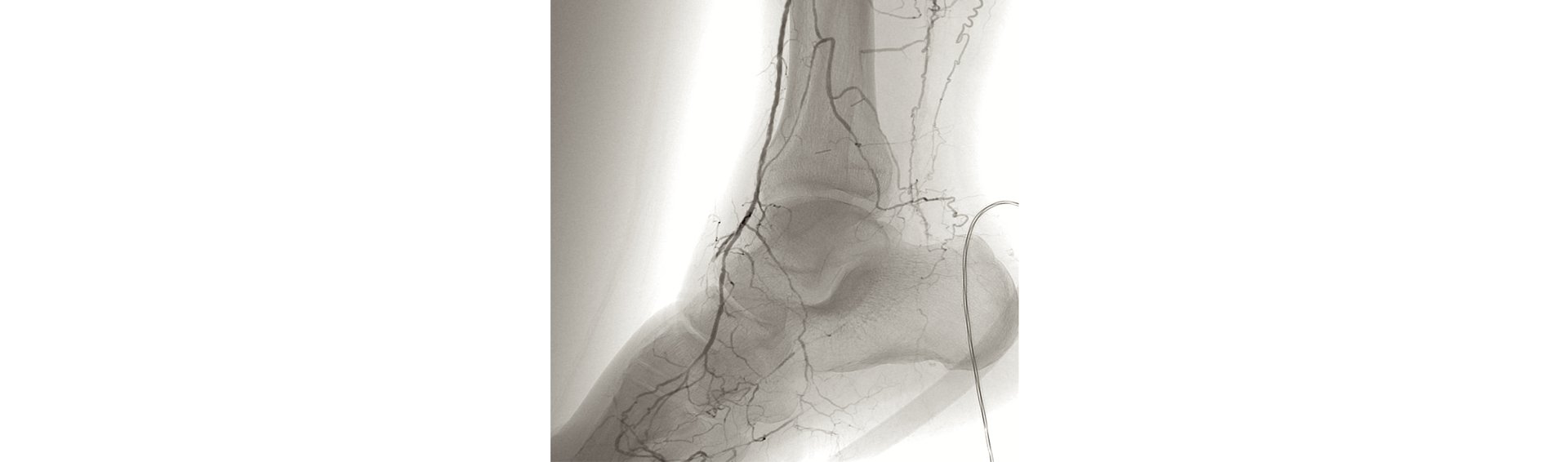
 PAOD is almost exclusively caused by arteriosclerosis.
PAOD is almost exclusively caused by arteriosclerosis.
The term is derived from ancient Greek and translates as ‘hardening of the arteries’. In the everyday language, “vessel calcification” is also common. In fact, calcifications can actually form in the peritoneal artery during the course of the disease, which can even be visible in x-ray images. The precise mechanism is not yet fully understood and remains a subject of research. At the beginning of the course of the disease, damage occurs in the inner cell lining of the artery, the endothelium. Subsequently, so-called ‘macrophages’ (devouring cells) enter the vessel wall, where cholesterol (blood fat) is stored, decay and eventually die off. This triggers an inflammatory response and sets repair mechanisms of the body is in motion. As a result, the blood clotting (coagulation) cascade is initiated, a gradual step-by-step process, is activated, resulting in local blood clotting and further narrowing of the vessel. Narrowings of the femoral (leg) arteries can lead to circulatory disorders, which can also lead to the loss of a leg. The main goal of treatment is the improvement of blood circulation.
A) Risk factors for PAOD
Smoking is a major risk factor for the development of peripheral arterial occlusive disease.There are almost no patients with a PAOD who do not smoke, or have no history of being a smoker. Other factors encouranging the development of PAVK are high blood pressure (hypertension), lack of exercise, being overweight, vitamin D3 deficiency and hypercholesterolaemia (excessive blood fats).
B) Symptoms of PAOD
The symptoms of PAOD are classified into different stages according to severity (‘Fontaine classification’):
Stage I
At this stage, arteries consist of narrowings, which are detectable by ultrasound or CT (computed tomography). However, these narrowings remain unnoticed by the patient – otherwise said, they do not cause symtoms yet.
Stage II
This is where leg cramping occurs while walking. The degree of discomfort, as well as a determination of appropriate therapeutic measures, should be medically examined on the basis of a 200m step-test. As a rule, artery narrowings are treated with a change of lifestyle and medication, so long as a the test is passed pain-free. If the pain-free walking distance is shorter than 200m, conventional treatment is not sufficient and must an advance must be made to invasive treatment such as surgery or endovascular treatment (see below), depending on the findings.
Stage III
A characteristic of this stage is pain at rest. These typically occur at night while lying down. Causes of this particular pain are pronounced vasoconstrictions, which affect several levels of the vascular system. Often the pain at rest can only be treated by a complex operation. From this stage onwards, a critical flow disturbance prevails which, in principle, is associated with the risk of the loss of limbs.
Stage IV
In stage IV, a loss of tissue in the area of the sole of the foot has already occurred – either by a non-healing, worsening wound (for example, after a pedicure), or by an ulcer (by cause of a skin defect that can penetrate to the bone). Without therapy, more and more tissue will be lost. In addition, the risk of an infection all the way up to blood poisoning is high. Treatment must start immediately. All existing treatment options (surgery, endovascular therapy, blood flow promoting infusions and antibiotic therapy) are to be used.
PAOD in diabetics
Patients with diabetes are particularly vulnerable to PAOD.
Often, they have already suffered damage to the sensitive nerves caused by the long-standing increased levels of blood glucose. Therefore, they do not feel any pressure points on the feet caused by too-tight shoes. In addition, bad or incorrectly controlled diabetes damages microscopic blood vessels (arteriolosclerosis). The blood flow condition is critical.
The treatment of diabetics with PAOD is complex and requires a great deal of patience and perseverance from both the patient and the treating physician.
C) Diagnosis of PAVC
Cramps and pain while walking are symptoms of PAVC: intermittent claudication or Charcot’s syndrome – temporary limping. Based on the state of the pulse – sensing the pulse – the area of the vascular constriction can already be confined. Furthermore can an analysis of the blood flow, by means of ultrasonic imaging, give further indications regarding the specific localization. For operational or interventional planning, medical imaging by virtue of contrast-enhanced computer tomography (CT angiography) or a magnetic resonance tomography (MRT angiography) is necessary.
D) Invasive treatment of PAOD
Narrowing of the arteries can usually be treated by balloon dilatation and stent implantation. A balloon dilatation is an operative measure, in which a catheter is introduced into the artery through a hypodermic needle, carrying an inflatable balloon. The balloon can be inflated with high pressure, so to expand a narrowed blood vessel (vasoconstriction). In most cases, a specifically designed wire mesh grid (stent) is inserted to secure the resulting outcome, which is placed keep the vessel open. Longer or larger closures are bridged with a bypass (collateral circuit). The great saphenous vein (a large vein that runs under the skin on the side of the leg) or plastic vascular prostheses can be used as a bypass material. In some cases, the small saphenous vein (which runs under the skin of the lower side of the thigh) is used as bypass material. Although rarely, even veins of the arm (cephalic or basilic vein) can be used. Vasoconstrictions or short narrowings/occlusions in the femoral arteries are treated by endartectomy. The plaque (deposition in the vessel) is peeled or scraped off with a special instrument (spatula) and the vessel incision extended by a patch. Here too, a vein, plastic or bovine pericardium (modified pericardial bovine tissue) can be used for the to be sewn-in patch.
E) Aftercare
Even it comes to aftercare, the point of convergence remains the reduction of any risk factors of atherosclerosis, and to thusly, also treat any other possible narrowings or vasoconstrictions. Clinical follow-ups of the arteries should be carried out every six months by means of a medical examination (by ultrasound, or as required) as well as the testing of blood lipid and vitamin D3 levels. Furthermore, nicotine may not be consumed.